undefined
undefined
By undefined · Updated undefined
Table of Contents
- Why Cats Hide Pain: Understanding Feline Instincts
- Behavioral Signs Your Cat Is in Pain
- Physical Signs: What to Look For on the Body
- The Feline Grimace Scale: A Scientifically Validated Tool
- Common Sources of Pain in Cats
- How to Assess Your Cat's Pain at Home
- Veterinary Approaches to Feline Pain Management
- Preventing Pain: Proactive Cat Care
- Frequently Asked Questions
- Sources & Methodology
Why Cats Hide Pain: Understanding Feline Instincts
To recognize pain in cats, you first need to understand why it is so difficult to detect. Unlike dogs — who have evolved alongside humans for tens of thousands of years and developed expressive communication — cats remain fundamentally wild animals within our homes. Their ancestor, Felis silvestris lybica (the African wildcat), survived by avoiding predator attention. A visibly injured cat signals vulnerability, and in the wild, that means death.
This survival instinct did not disappear through domestication. It merely adapted. Your well-fed, indoor cat still carries the same neurological and hormonal responses as her wild ancestors. When pain begins, the first and most consistent feline response is to retreat and hide. You may notice your cat disappearing under the bed, into a closet, or behind furniture — not because they are being antisocial, but because they are responding to a deep, biological imperative to protect themselves from perceived threats.
Compounding this is the cat's unique pain expression. Where a human might groan, cry, or point to a painful area, a cat's outward signs are far more nuanced. Cats rarely vocalize pain unless it is severe or sudden (such as acute trauma). More commonly, pain manifests as quiet behavioral changes — a cat who once greeted you at the door now staying in one room, a formerly social cat becoming aggressive when touched, or an avid groomer suddenly looking unkempt.
Understanding this context is essential because it means the burden of detection falls almost entirely on you, the owner. You are the one who sees your cat daily, who knows their routines, their favorite spots, and their unique personality quirks. No one else is positioned to notice the small deviations that could indicate significant pain.
Behavioral Signs Your Cat Is in Pain

Behavioral changes are typically the earliest and most reliable indicators that something is wrong. Unlike physical symptoms, which may not become apparent until a condition has progressed, behavioral deviations often emerge within hours of pain onset.
1. Increased Hiding and Withdrawal
One of the most universal signs of pain in cats is prolonged hiding. While it is normal for cats to seek quiet rest spots, a cat in pain will often choose the most secluded location available — behind the couch, at the back of a closet, under the bed in the furthest corner. They may emerge only to eat or use the litter box, if at all. If your social, curious cat suddenly becomes a ghost in your home, treat this as a serious red flag requiring investigation.
2. Changes in Vocalization
A cat's voice is a remarkably sensitive instrument. Pain-related vocalization can manifest in several ways:
- Increased meowing or yowling, especially at night or in quiet environments
- New sounds your cat has never made before — honking, growling, or chattering
- Decreased vocalization in cats who were previously chatty (some cats respond to pain by going silent rather than becoming louder)
- Groaning or whimpering during movement or when being picked up
Any significant change in your cat's vocal patterns — in either direction — warrants a closer look. For more on understanding feline communication, see our cat behavior guide.
3. Aggression or Irritability When Touched
Pain makes cats defensive. A gentle cat who suddenly bites, scratches, hisses, or growls when you pet them or pick them up is likely experiencing pain. This is especially common when the painful area is near the point of contact. Cats with dental disease, for example, may become aggressive around their face or mouth area, while cats with back or hip pain may react violently to being stroked along the spine or lifted.
Never punish a cat for aggressive behavior during pain — they are not being "mean." They are communicating the only way they can.
4. Reduced Grooming or Over-Grooming
Cats typically spend 30–50% of their day grooming when healthy. Pain disrupts this routine in two ways:
- Under-grooming: A cat in pain lacks the energy and flexibility to maintain their coat. Their fur becomes matted, greasy, or dull. This is especially common in cats with arthritis who cannot twist to reach their lower back or hindquarters.
- Over-grooming: Conversely, some cats lick a painful area obsessively, creating bald patches, raw skin, or hot spots. This is a self-soothing behavior that can actually worsen skin damage over time.
Both scenarios are abnormal and should prompt a veterinary visit. For tips on maintaining your cat's coat between vet visits, read our cat grooming tips.
5. Changes in Appetite and Thirst
Pain suppresses appetite in nearly all animals, and cats are no exception. You may notice your cat walking to their food bowl but not eating, eating only a few bites, or ignoring their favorite foods entirely. Inappetence lasting more than 24 hours is a medical emergency in cats because it can rapidly lead to hepatic lipidosis (fatty liver disease).
Some cats may also drink less water when in pain, leading to dehydration. Monitor your cat's water bowl and note how much they are drinking each day.
6. Litter Box Avoidance or Changes
Pain can affect litter box habits in several ways:
- Avoiding the litter box due to pain during entry, exit, or the physical act of urinating/defecating (common in cats with urinary tract infections or constipation)
- Changes in urine or stool — straining, crying during elimination, blood in urine or stool, diarrhea, or constipation
- Going outside the litter box — this is not spite; it is often a distress signal indicating pain makes it difficult to reach or use the box in time
If your cat eliminates outside the box, schedule a vet appointment before assuming a behavioral problem. Our cat litter box guide covers proper box setup and when to be concerned.
7. Restlessness and Inability to Settle
A cat in pain may pace, repeatedly get up and lie down, shift positions constantly, or appear unable to find a comfortable resting spot. They may sleep in unusual positions — hunched over, pressed into a corner, or with their head tucked under a paw for hours at a time.
8. Neglecting Favorite Activities
If your cat stops playing, climbing, or using their cat tree, it could indicate pain. Cats are driven by routine, and the loss of preferred activities — especially in an otherwise healthy-seeming cat — is a meaningful signal that deserves attention.
Physical Signs: What to Look For on the Body

While behavioral signs are often subtle, physical indicators can be more immediately apparent if you know what to look for. Conduct a weekly gentle physical inspection of your cat — running your hands over their body, checking their face, paws, and coat — and watch for the following:
Posture and Gait
- Hunched posture: A healthy cat at rest may curl up or stretch luxuriously. A cat in pain often sits in a tight, compact ball with their head lowered or tucked — maximizing warmth and minimizing the energy required to hold themselves upright.
- Lameness or limping: Favoring one or more legs is an obvious sign but can be subtle in early stages. Watch for reluctance to jump, shortened stride, or a "hopping" gait when descending from heights.
- Head tilt: May indicate inner ear infection or neurological pain.
- Reluctance to fully extend limbs: Cats with joint pain often keep their legs slightly bent even when standing.
Eye Changes
The eyes are exceptionally expressive in cats. Watch for:
- Squinting or half-closed eyes (orbital tightening — a core component of the Feline Grimace Scale)
- Unequal pupil sizes (anisocoria) — can indicate neurological pain or trauma
- Dull or glazed appearance
- Third eyelid showing (the nictitating membrane partially covering the eye) — this is never normal in a resting, alert cat and indicates either pain, illness, or injury
- Excessive tearing or discharge
Breathing Changes
Rapid, shallow breathing or open-mouth breathing in a cat is a medical emergency. While dogs may pant from heat or stress, cats almost never open their mouths to breathe casually. If your cat is breathing with their mouth open, seek emergency veterinary care immediately. Labored breathing, wheezing, or a visible increase in respiratory rate at rest are all urgent warning signs.
Mouth and Dental Signs

Dental disease is one of the most common sources of chronic pain in cats. Inspect your cat's mouth gently (only if safe for you to do so) and look for:
- Red, swollen, or bleeding gums
- Broken, missing, or discolored teeth
- Excessive drooling
- Dropping food from the mouth while eating
- Pawing at the mouth
- Foul breath (not normal in cats — contrary to popular belief)
Annual dental checkups are critical. Our guide to cat nutrition also covers foods that support oral health.
Coat and Skin Condition
As noted above, grooming disruptions cause visible coat deterioration. Additionally:
- Visible injuries: Cuts, wounds, swelling, or bruises — even small wounds can be intensely painful
- Bloating or distended abdomen: Could indicate internal pain from organ enlargement, fluid retention, or obstruction
- Visible ribs or spine: Sudden weight loss is always a concern and often accompanies chronic pain
Tail and Limb Responses
- Tail flicking or tucking: A tucked tail often signals fear or pain
- Pain response when touching specific areas: If your cat flinches, cries, or withdraws when you touch a particular spot, that area deserves immediate veterinary attention
- Numbness or weakness in hind legs: Often seen in cats with aortic thromboembolism or advanced spinal disease — this is an emergency
The Feline Grimace Scale: A Scientifically Validated Tool
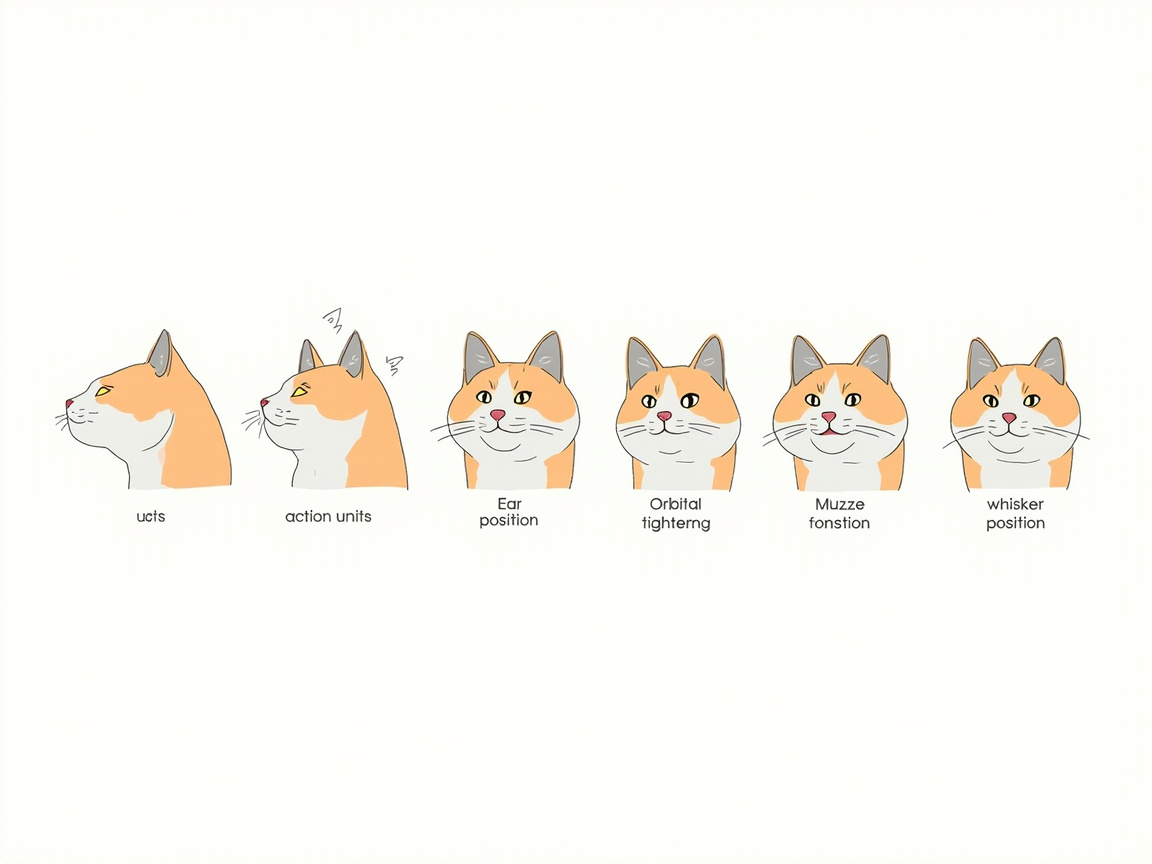
The Feline Grimace Scale (FGS) is a scientifically validated pain assessment tool originally developed by researchers at the University of Montreal and now endorsed by the International Society of Feline Medicine (ISFM). It provides an objective, repeatable method for both veterinarians and cat owners to score pain levels based on five facial action units.
Unlike subjective assessments, the FGS has been tested in clinical settings and demonstrates strong reliability. It is particularly useful for detecting post-operative pain and pain from acute conditions, and serves as a valuable communication tool between you and your veterinarian.
The Five Action Units
Each unit is scored 0 (absent), 1 (moderate/uncertain), or 2 (obvious). The scores are summed to produce a total between 0 and 10.
| Action Unit | Score 0 (Absent) | Score 1 (Moderate) | Score 2 (Obvious) |
|---|---|---|---|
| Ear Position | Ears pointing forward, relaxed | Ears slightly pulled back | Ears flattened firmly against the head |
| Orbital Tightening | Eyes open, relaxed | Slightly squinted or narrowed | Eyes tightly closed or half-closed |
| Muzzle Tension | Muzzle relaxed, rounded | Slightly tensioned, oval | Muzzle clearly tense, elliptical, whiskers forward |
| Whisker Position | Whiskers loose, curved | Whiskers slightly stiffened | Whiskers straight, rigid, bunched forward |
| Head Position | Head up, alert | Head slightly lowered | Head down, below shoulder line, tilted |
How to Score
- Observe your cat from approximately one meter away, ideally when they are resting but awake (not purring excessively, not sleeping deeply).
- Score each action unit independently.
- Add all five scores for a total score.
- A score of 4 or above indicates significant pain requiring veterinary consultation and potentially analgesia.
Important Caveats
- The FGS is most reliable for acute pain (injury, surgery). It is less validated for chronic pain conditions like osteoarthritis, where behavioral signs are more informative.
- Do not score your cat immediately after they have been startled or are highly alert — the baseline resting state is most informative.
- Use the FGS as one tool among many. Never rely on a single assessment in isolation.
- If your cat scores 4 or above, contact your veterinarian. If they score 7 or above, seek emergency care.
Research published in the Journal of Feline Medicine and Surgery (2019) confirmed the FGS as a reliable tool for detecting pain in cats, and the scale has since been incorporated into veterinary practice guidelines across North America and Europe.
Common Sources of Pain in Cats
Understanding what causes pain in cats helps you contextualize what you observe and communicate more effectively with your veterinarian. Below are the most prevalent pain conditions in domestic cats.
Dental Disease
Dental disease is the most common cause of chronic oral pain in cats. By age three, the majority of cats have some degree of periodontal disease. Beyond gum inflammation, cats suffer from:
- Tooth resorption lesions (FORL — Feline Oral Resorptive Lesions), which erode teeth from the root and are extremely painful
- Stomatitis — severe inflammation of the entire mouth, causing intense pain and inappetence
- Broken teeth from trauma or chewing on hard objects
Signs of dental pain include pawing at the mouth, drooling, chattering jaw, refusing dry kibble, and facial swelling. Our cat nutrition guide discusses the role of diet in dental health.
Osteoarthritis
Degenerative joint disease affects an estimated 30–60% of cats over six years of age, though only a fraction are diagnosed. Unlike dogs, cats rarely limp obviously. Instead, signs are behavioral:
- Reluctance to jump or climbing shorter distances
- Using furniture as a stepping stool rather than leaping directly
- Difficulty getting into the litter box (especially with high sides)
- Reduced grooming of the hindquarters
- Stiffness after rest
There is no cure for osteoarthritis, but pain management — including joint supplements, environmental modifications, and veterinary-prescribed medications — can significantly improve quality of life.
Urinary Tract Disorders
Painful urinary conditions are extremely common, especially in indoor, neutered male cats and middle-aged female cats. These include:
- Feline Idiopathic Cystitis (FIC): Inflammation of the bladder without known cause, causing intense pain during urination
- Urinary blockage: A life-threatening emergency in male cats where crystals or stones obstruct the urethra
- Bladder stones: Cause pain during urination and can lead to blockage
Signs include straining to urinate, crying during elimination, urinating outside the box, frequent small urinations, and blood in the urine. A completely blocked cat — unable to urinate — is a medical emergency requiring immediate veterinary care.
Gastrointestinal Pain
Inflammatory bowel disease (IBD), pancreatitis, constipation, foreign body obstruction, and gastroenteritis all cause significant abdominal pain. Watch for:
- Vomiting, especially if repeated or containing blood
- Diarrhea or constipation
- Distended or hard abdomen
- Pain when the abdomen is gently palpated (a veterinarian should do this)
- Weight loss and poor coat condition over time
Trauma
Trauma from falls (high-rise syndrome), vehicle accidents, animal bites, gunshot wounds, or household accidents is a major cause of acute pain in cats. Outdoor cats and cats in multi-pet households are at higher risk. Any suspected trauma warrants immediate veterinary evaluation — even if your cat appears to be walking normally, internal injuries may not be immediately apparent.
Post-Surgical Pain
Following any surgical procedure — from spay/neuter to dental extractions to tumor removal — cats require appropriate pain management. Your veterinarian should send your cat home with pain medication after any surgery. If your cat seems excessively lethargic, refuses food, or shows signs of discomfort after a procedure, contact your vet.
Cancer
While not all cancers cause pain, many do — either from tumor growth pressing on organs and nerves, or from the inflammatory processes cancer triggers. Early detection and management are critical for maintaining quality of life.
How to Assess Your Cat's Pain at Home

You do not need veterinary training to conduct a basic home pain assessment. Follow this step-by-step process at least weekly for adult cats and twice weekly for senior cats (7+ years) or cats with known health conditions.
Step 1: Observe From a Distance (2 Minutes)
Before touching your cat, sit quietly and observe:
- How are they breathing? Normal rate is 20–30 breaths per minute at rest.
- What is their posture? Loose, relaxed, or hunched and rigid?
- Are they in their usual resting spot, or somewhere unusual?
- Are both eyes open and bright? Any squinting?
- Is there any vocalization?
Step 2: Approach and Interact
Call your cat to you or offer a treat. Note their response:
- Do they come readily, or hesitate due to pain?
- Is their movement fluid or stiff?
- Do they favor any legs when walking?
- Are they purring? (Remember: purring does not exclude pain.)
Step 3: Physical Palpation
With clean hands and gentle pressure, run your hands over your cat's body:
- Head and face: Feel around the jaw, under the ears, and along the cheeks
- Neck and spine: Run your fingers along the spine from neck to tail base
- Ribs and chest: Gently feel the ribcage — check for any masses, wounds, or swelling
- Abdomen: Very gently — if the abdomen feels hard, tight, or your cat pulls away, this is a red flag
- Legs and paws: Flex and extend each leg gently; check between toes for injuries; inspect claws
- Tail: Check for wounds, swelling, or sensitivity near the base
Step 4: Use the Feline Grimace Scale
Apply the FGS scoring method described above. Record the score and date so you can track changes over time.
Step 5: Monitor Litter Box Habits
Keep a simple log of:
- Number of litter box visits per day
- Urination vs. defecation frequency
- Stool consistency (using a Fecal Scoring System for reference)
- Any straining, crying, or blood
- Location of eliminations (inside box or elsewhere)
Step 6: Track Weight Monthly
Use a baby scale or pet scale to weigh your cat monthly. Weight loss — even in an eating cat — is a serious indicator of underlying disease and pain. Unexplained weight loss of more than 10% warrants immediate veterinary investigation.
Veterinary Approaches to Feline Pain Management

When you bring your cat to the veterinarian for a pain evaluation, expect a multi-step diagnostic process. Understanding what happens at the vet's office helps you prepare and ensures you can provide the most useful information.
The Diagnostic Process
- Physical examination: Your veterinarian will conduct a thorough head-to-tail exam, including oral examination (often requiring sedation for a full oral evaluation), palpation of the abdomen and joints, and neurological assessment.
- History taking: Your veterinarian will ask detailed questions about behavior changes at home. Come prepared with your observations — bring notes from your home assessments if possible.
- Diagnostic testing: Depending on findings, your vet may recommend bloodwork, urinalysis, X-rays, ultrasound, or advanced imaging (CT/MRI) to identify the source of pain.
- Pain scoring: Your vet may use the FGS, a numerical rating scale, or a visual analogue scale to quantify your cat's pain level before and after treatment.
Common Pain Medications for Cats
| Medication | Type | Common Uses | Notes |
|---|---|---|---|
| Meloxicam (Metacam) | NSAID | Post-surgical, osteoarthritis, acute pain | Single-dose or short-term use; nephrotoxic if overdosed |
| Buprenorphine | Opioid partial agonist | Moderate to severe pain, post-surgical | Commonly used in practice; administered transmucosally |
| Gabapentin | Anticonvulsant/neuropathic agent | Nerve pain, chronic osteoarthritis, anxiety-related pain | Often well-tolerated; sedating effect is common |
| Tramadol | Opioid analgesic | Moderate to severe pain | Used cautiously; can cause serotonin syndrome in some cats |
| Amantadine | NMDA antagonist | Chronic cancer pain, severe osteoarthritis | Typically used in combination therapy |
| Corticosteroids (e.g., prednisone) | Anti-inflammatory | Inflammatory conditions, autoimmune pain | Used short-term; long-term use has significant side effects |
Crucially, never give your cat any medication without explicit veterinary instruction. The wrong drug or dose can cause organ failure, gastrointestinal ulcers, or death.
Non-Pharmacological Approaches
Modern feline pain management extends beyond medications:
- Acupuncture: Feline acupuncture by a certified veterinary acupuncturist has shown promise for chronic pain conditions, particularly osteoarthritis
- Physical therapy and rehabilitation: Techniques including passive range-of-motion exercises, laser therapy, and hydrotherapy
- Environmental modification: Providing orthopedic beds, lowering food bowls, adding ramps to favorite perching spots, and using low-sided litter boxes
- Weight management: Excess weight places additional strain on joints and worsens arthritis pain
- Joint supplements: Products containing glucosamine, chondroitin, and omega-3 fatty acids may support joint health (consult your vet before starting any supplement)
If you have an older cat struggling with mobility, consider an elevated cat feeder or orthopedic cat bed to reduce strain during eating and resting. These simple environmental changes can make a meaningful difference in comfort without any medication.
When to Seek Emergency Care
The following symptoms indicate your cat needs immediate veterinary or emergency care:
- Open-mouth breathing or labored breathing
- Complete refusal to eat for more than 24 hours
- Inability to urinate (especially male cats — this is life-threatening)
- Sudden paralysis of the hind legs
- Visible severe injury or profuse bleeding
- Extreme aggression suggesting severe pain
- Collapse or inability to stand
- Seizures
- Signs of shock (pale gums, rapid breathing, cold extremities)
Preventing Pain: Proactive Cat Care

While not all pain is preventable, a proactive approach to your cat's health dramatically reduces the risk of many painful conditions and catches others early when they are most treatable.
Regular Veterinary Checkups
Cats should see a veterinarian at least once per year for a wellness exam. For cats over seven years of age, twice-yearly exams are strongly recommended. Many serious conditions — including dental disease, kidney disease, hyperthyroidism, and cancer — can be detected during routine screening before they cause significant pain.
Our guide to cat vet checkups covers what to expect at each life stage and how to prepare for your appointment.
Dental Care
Daily brushing is the gold standard for preventing dental disease. Use a cat-specific toothbrush and enzymatic feline toothpaste — never use human toothpaste. If your cat tolerates brushing, you can dramatically reduce the risk of periodontal disease, the most common source of oral pain in cats.
For cats who won't tolerate brushing, dental treats, water additives, and prescription dental diets can help, though they are not substitutes for brushing.
Weight Management
Obesity is a major risk factor for joint pain, diabetes (which causes generalized pain), hepatic lipidosis, and numerous other conditions. Feed a balanced, species-appropriate diet and monitor portion sizes carefully. Our cat nutrition guide covers calorie requirements, reading pet food labels, and choosing the right diet for your cat's life stage.
Safe Environment
Eliminate hazards that could cause traumatic injury:
- Secure windows with sturdy screens (prevent falls)
- Keep toxic plants (lilies, sago palms, azaleas) out of the home
- Store medications, chemicals, and small objects that could be swallowed out of reach
- Provide appropriate scratching surfaces to prevent claw damage
- Use cat-safe cleaning products
Parasite Prevention
Flea infestations cause intense itching and skin pain. Tick-borne diseases can cause joint pain and neurological symptoms. Use veterinarian-recommended parasite prevention products year-round, even for indoor-only cats.
Know Your Cat's Baseline
The single most effective pain-detection tool available to you is knowing your cat. Understand their daily routine, personality, favorite spots, typical vocalization patterns, and normal activity levels. Any deviation from their established baseline is worth noting and, if persistent, investigating.
Keep a simple journal or use a pet health tracking app to log your cat's eating, drinking, grooming, and activity. Patterns in this data can reveal pain long before it becomes obvious.
Frequently Asked Questions
How do I know if my cat is in pain or just tired?
Pain in cats is persistent and often accompanied by additional signs such as hiding, reduced grooming, aggression, or changes in eating and litter box habits. Fatigue is temporary and your cat will return to normal behavior once rested. If behavioral changes last more than 24–48 hours, consult a veterinarian.
What is the Feline Grimace Scale and how do I use it?
The Feline Grimace Scale (FGS) is a scientifically validated tool that scores five facial action units: ear position, orbital tightening, muzzle tension, whisker position, and head position. Each is scored 0 (absent), 1 (moderate), or 2 (obvious). A total score of 4 or above indicates significant pain requiring veterinary attention.
Can cats fake being in pain?
Cats cannot deliberately fake pain in the way humans might. However, pain-driven behavioral changes — such as excessive vocalization or aggression — can appear manipulative but are genuine responses to discomfort. Always assume pain is real and seek veterinary evaluation rather than dismissing it as behavioral.
Should I give my cat human pain medication?
Never. NSAIDs like ibuprofen (Advil) and naproxen (Aleve), as well as acetaminophen (Tylenol), are toxic to cats and can cause acute kidney failure or death. Even a single dose can be fatal. Only pain medications specifically prescribed by your veterinarian are safe for cats.
When should I take my cat to the vet for pain?
Take your cat to the vet immediately if they show any of the following: refusal to eat for more than 24 hours, difficulty breathing, complete hiding for more than a day, sudden aggression toward touch, inability to use the litter box, visible injury, pale gums, collapse, or a Grimace Scale score of 4 or above.
What are the most common causes of pain in indoor cats?
The most common pain sources in cats include dental disease, osteoarthritis, urinary tract infections and blockages, pancreatitis, inflammatory bowel disease, trauma from falls or accidents, post-surgical recovery, and cancer. Senior cats (7+ years) are at higher risk for degenerative conditions like arthritis.
Do cats purr when they are in pain?
Yes. Cats purr for many reasons, including self-soothing when injured or unwell. While purring often indicates contentment in healthy cats, it can also be a coping mechanism during pain or illness. Never rely on purring alone as a sign your cat is fine — always evaluate other behavioral and physical signs together.
My cat is limping but seems fine otherwise. Should I wait to see if it gets better?
Limping always indicates pain and should never be ignored. If your cat is limping, schedule a veterinary appointment within 24–48 hours. If the limping is severe, accompanied by swelling, an open wound, or your cat is not bearing any weight on the limb, seek emergency care immediately. Early intervention dramatically improves outcomes for musculoskeletal injuries.
Sources & Methodology
This article was researched and written according to the following standards and sources:
-
Feline Grimace Scale Validation Study — Evangelista MC, et al. Journal of Feline Medicine and Surgery (2019). "Facial expressions of pain in cats: the development and validation of a Feline Grimace Scale." https://journals.sagepub.com/doi/10.1177/1098612X19839544
-
International Society of Feline Medicine (ISFM) Pain Management Guidelines — ISFM Consensus Guidelines on the Management of Pain in Cats. Journal of Feline Medicine and Surgery (2022). https://journals.sagepub.com/doi/10.1177/1098612X221128357
-
AAFP Feline Pain Management Guidelines — American Association of Feline Practitioners. Journal of Feline Medicine and Surgery (2023). https://catvets.com/public/pdfs/guidelines/AAFP_Pain_Management_Guidelines.pdf
-
WSAVA Global Dental Guidelines — World Small Animal Veterinary Association. Feline oral health guidelines for standardizing dental care. https://www.wsava.org/GlobalGuidelines
-
AAHA Canine and Feline Pain Management Guidelines (2022 revision) — American Animal Hospital Association. https://www.aaha.org/
-
Feline Osteoarthritis Prevalence Study — Slingerland LI, et al. Veterinary Journal (2021). Cross-sectional study of radiographic osteoarthritis prevalence in cats. https://www.sciencedirect.com/science/article/pii/S1090023319302203
-
Cornell University College of Veterinary Medicine — Feline Health Center. Pain recognition and management resources. https://www.vet.cornell.edu/departments-centers-and-institutes/cornell-feline-health-center
-
University of Edinburgh Royal (Dick) School of Veterinary Studies — Pain assessment in companion animals. Research into feline pain expression and quantification.
-
AVMA Guidelines for Veterinary Pain Management — American Veterinary Medical Association. https://www.avma.org/
-
Feline Lower Urinary Tract Disease (FLUTD) Overview — Hostutler RA, et al. Veterinary Clinics: Small Animal Practice (2020). https://www.sciencedirect.com/science/article/pii/S0195561620300211
About the Author
Rachel is a Certified Feline Behavior Specialist with over a decade of experience working with domestic cats in clinical, shelter, and home consultation settings. She holds credentials from the International Association of Animal Behavior Consultants (IAABC) and has contributed to feline welfare research with the ASPCA. Her work focuses on helping cat owners understand and respond to feline behavioral and medical cues before problems escalate. She shares her home with three rescue cats: Miso, Fig, and Pemberton.
Last updated: April 2026. This article is reviewed annually or when significant new veterinary research is published.